World Breastfeeding Week - Sustaining Breastfeeding Together
TUESDAY, AUGUST 04, 2020
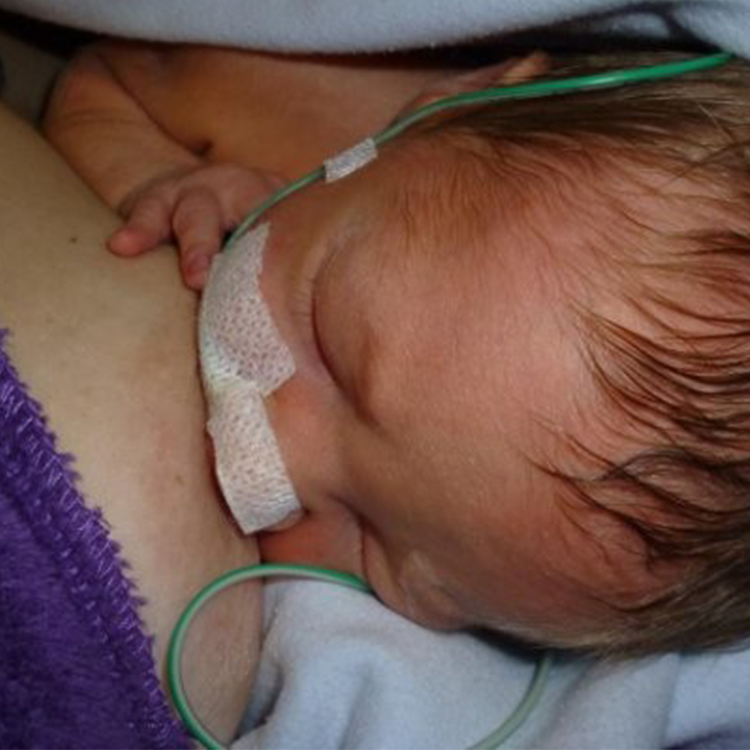 Before your baby is born, you spend time imagining their birth and how you would care for them. You may have even spent time thinking about how you planned to feed your little one after their arrival. When your baby is born premature or sick and admitted to a Neonatal Intensive Care Unit (NICU) or Special Care Nursery (SCN), you find yourself needing to adjust your dreams and expectations.
Before your baby is born, you spend time imagining their birth and how you would care for them. You may have even spent time thinking about how you planned to feed your little one after their arrival. When your baby is born premature or sick and admitted to a Neonatal Intensive Care Unit (NICU) or Special Care Nursery (SCN), you find yourself needing to adjust your dreams and expectations.
The World Health Organization (WHO) recognises breastmilk as the best nutritional food source for newborns as it is vital for the healthy growth and development of infants. It also has important implications for the health of new mothers. Both WHO and UNICEF recommend that breastfeeding should be initiated within one hour of a baby’s birth and should continue during the first six months of the child’s life and ideally until the age of two.
But what happens when your baby is born too early to yet know how to suck, swallow and breathe or too sick to feed from the breast?
You are thrown into an exhausting new world of hand-expressing every 3 hours during those first few days before being moved to a pump where you could find yourself for days or weeks on end trying to provide milk for your little one who remains in critical care.
“My baby was born at 26 weeks, and I expressed for the first 9 weeks and had enough milk to get me to special care when I stopped expressing. I was exhausted and mentally unstable. Setting an alarm in the night to get up and attach a machine to my breast (and not my baby) and imagine what he was doing (in hospital) the whole time was unbearable for me.” Miracle Mum (name protected at mothers request)
Tube Feeding
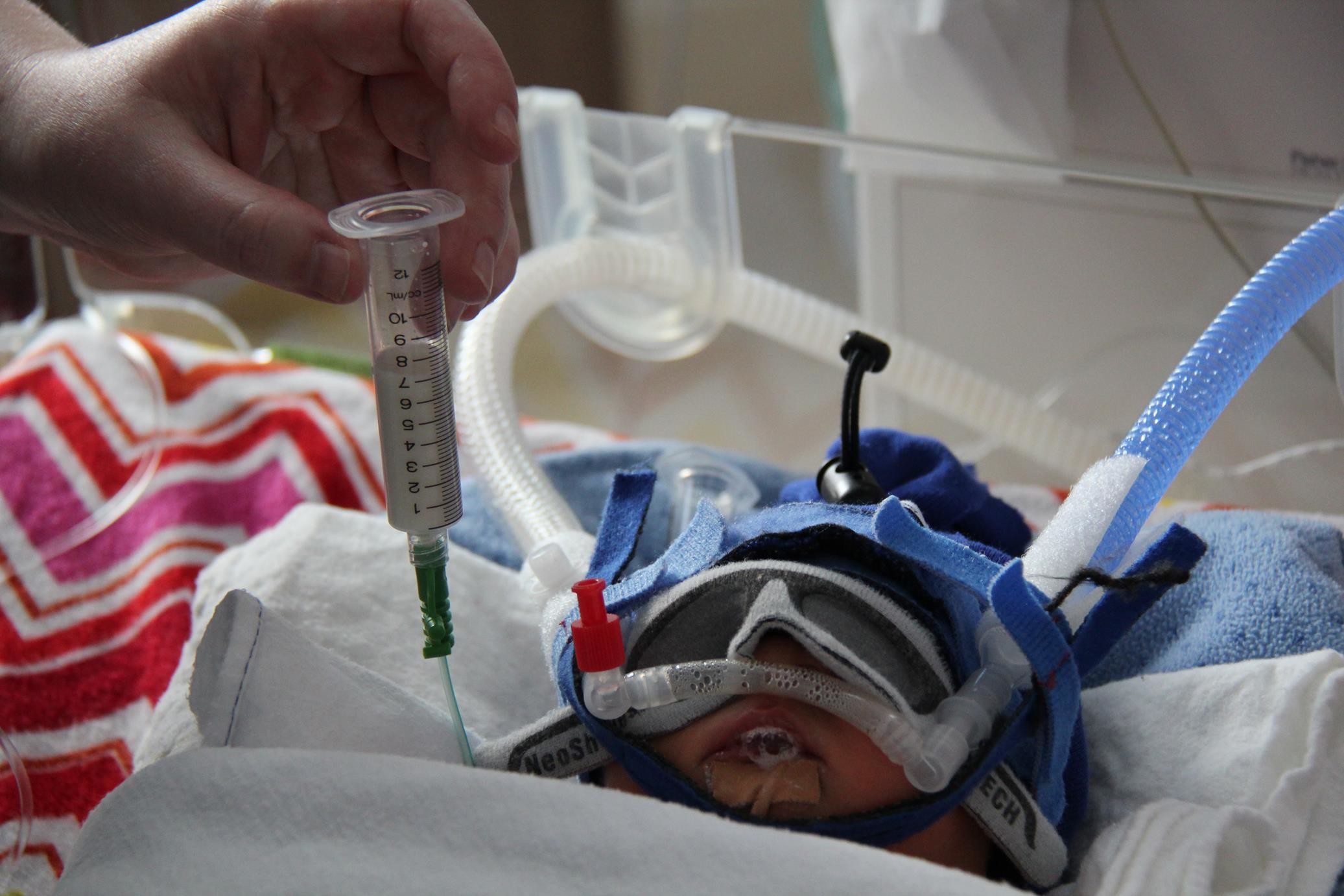
Generally, a premature baby’s digestive system is ready for milk feeds before they are actually able to coordinate all the muscles needed for sucking, swallowing and breathing.
In order to receive the milk, a small thin tube called a naso-gastric tube (NG tube) is passed through their nose or mouth, and down into their stomach. The baby’s feed can then be pushed down the tube with a syringe or sometimes an electric pump may be used to continuously allow the milk down.
Why is breastmilk so important for premature and sick babies?
Breast milk is important for all babies but for premature and sick newborns, it provides vitally important health benefits and acts like a medicine that only mothers milk can provide. Research has shown that the composition of a mother’s breast milk is different if her baby is born premature than if her baby was born fullterm. It is tailored to the needs of a premature gut and is highly beneficial for baby.
The longer a premature or sick baby has access to breastmilk, the more profound and long-lasting the benefits.
- Breast milk provides better nutrient absorption, digestive functioning and nervous system development.
- Colostrum (first milk) is rich in antibodies called ‘immunoglobins’ and coats the gastro-intestinal tract, stomach and intestines, providing protection from viruses and bacteria.
- Mothers of premature babies produce milk that is higher in nitrogen, protein, lipids, fatty acids, vitamins, calcium and other vital elements that are important to the development of premmies.
- Breast milk antibodies protect from viruses such as gastroenteritis, sepsis and necrotising enterocolitis.
- Research shows that breast milk reduces the risk of conditions such as allergies, asthma and eczema.
- The varying composition of breast milk keeps pace with the baby’s changing nutritional needs.
- Breast milk has vital long-chain polyunsaturated fatty acids, which are essential to brain development.
New mothers need continued emotional support to build not only establish an initial supply but to continue during lengthy hospital stays and also in making the transition from expressing to feeding the baby at the breast.
Providing for others
To support those mothers and babies who do not have access to their mother’s own milk, human milk banks will continue to play a vital role in the care of our countries most vulnerable babies. It is the right of every baby being cared for in a NICU or SCN to have access to their mother’s own milk or donor milk - the only milk that has been designed specifically by nature to give them the best help when they are at such a high risk of serious complications or sadly, death.

“I just wanted to share this picture. This was the last lot of milk I donated to the milk bank (in Perth). I donated 3 times over 7 weeks. My son was born at 23+5 weeks and sadly passed away at 3 days old. I decided, instead of dumping my large milk supply I would pump for other micro prems.” Miracle Mum, Jessica (shared on the Miracle Babies Foundation Facebook page)
World Breastfeeding Week is held annually between the 1st – 7th of August to encourage breastfeeding and improve the health of babies around the world.
This years theme is “support breastfeeding for a healthier planet”. In line with this theme, WHO and UNICEF are calling on governments to protect and promote women's access to skilled breastfeeding counselling, a critical component of breastfeeding support.
For support in Australia, contact:
Miracle Babies Foundation
1300 662 243 (24hour NurtureLine)
Australian Breastfeeding Association
1800 686 268
To donate breastmilk, contact:
LifeBlood MilkBank
1300 459 040


